We must weigh risks based on accurate information and take appropriate precautions.
Related Posts
Summary: Eventually, SARS-CoV-2 will move from a pandemic to an endemic state, but it will not be like an on/off switch. It may take a while, because many people globally and in the United States remain unvaccinated, thus eliminating the opportunity for a faster ending. We must learn to live with SARS-CoV-2 and the risk of infection. That means daily assessing which risks we are willing to bear and which we most want to avoid. Most of us who must work, manage households and go to school have to accept some level of risk. If we have accurate information and take all appropriate precautions, we can feel some sense of agency and get comfortable with the discomfort of ambiguity. Some people will have to weigh risks much more cautiously, for example, those who have children too young to be vaccinated, or older or other at-risk people in the home. But most of us cannot slam the door on the pandemic. We’ve got to venture out, however cautiously, managing risk and fear. The virus is all over the place. We must learn to live with it and do our best to outsmart it by being vaccinated and wearing masks. At the end, I provide a resource for coping in uncertain times from Krista Tippett, creator and host of the “On Being” public radio program and podcast.
First, we hoped for an end to the pandemic, but it hasn’t happened yet.
There was a time when we thought and hoped that we could vaccinate our way out of the pandemic. In the weeks after the first two vaccines received emergency use authorization, we logged onto websites and frenetically searched for appointments, and people like me were willing to drive hours to get vaccinated (without jumping the line). President Biden envisioned Independence Day celebrations with family at a time when 70% or more of the U.S. population would be vaccinated. But somewhere on the way to the dream of herd immunity, which we no longer talk as much about, something happened. The crowds at vaccination sites slowed to a trickle. Governors and others began to offer big and small financial inducements to people to get vaccinated. Slowly, increases began in some states, but others remained stalled. Some governors, such as Ron DeSantis of Florida and Greg Abbott of Texas, forbade policies, such as masking and vaccination, that would have helped to prevent the surges their states now are experiencing.
Jonathan Metsch, DrPH, clinical professor of environmental medicine and public health at Icahn School of Medicine at Mount Sinai, who curates and posts COVID-19 information regularly, recently highlighted another state, South Dakota.
The infamous and popular tradition known as the Sturgis Motorcycle Rally will gather (700,000) bikers as they cruise through the countryside from August 6 to August 15. (See Outsider.com.) Governor Kristi Noem of South Dakota, posting on Facebook, said: “The Sturgis rally is about hopping on your bike and exploring this great country through our open roads. Bikers come here because they WANT to be here. And we love to see them! There’s a risk associated with everything that we do in life. Bikers get that better than anyone.”
Metsch went on to say that the pandemic will end, as all pandemics do, but the virus probably will become endemic. Depending on the type of immune response the virus engenders, it could become endemic faster, with most cases mild. We must live with the pandemic until it drifts into an endemic state, as described by Jennie Lavine, et al, in Science. This will not be like watching a movie and seeing The End. We may not even be fully aware of the transition, but it is not happening in the next several months. (Also see Stat.) That means we must learn to live with it. We must co-exist.
“There is no one definition of what the end of a pandemic means,” Metsch wrote. (See NPR.) “The question of when the crisis will be over is a layered one — with different answers from local, national and global perspectives.” (See National Geographic.)
Reflecting on the global perspective, The New York Times recently reported,
In Spain and Britain, where vaccine supplies are ample, cases have begun declining after the Delta variant drove numbers to concerning heights. But in other countries like Malaysia and Thailand, where doses are more scarce, that climb is continuing. In the United States, with about 93 million people eligible for shots who have chosen not to get them, experts say that a rise in cases this winter is inevitable.
Most models predict increases in cases before they begin to decline sometime in October in the U.S.
Learning to live with a deadly agent in our midst
It’s not easy to live with a deadly agent that could be anywhere — in the sneeze of a stranger, the cough of a loved one, the breath of a patient or our dining companion. If we stop to think about all the ways we could be attacked, it is depressing, threatening and potentially immobilizing. So, we’ve got to use the tools we have — vaccination, masking, sound information and our own individual risk assessments. Among vaccinated people, the chances of getting the virus are much lower, and the chances of ending up hospitalized or dying are incredibly low even if there are some breakthrough infections. Most of us cannot stay inside our homes until this is over, and it is not going to be over soon. We lost that chance when the Delta variant got a foothold in this country due to a substantial portion of the population not getting vaccinated, and many people still not wearing masks. I am not blaming the unvaccinated. Nor am I making light of people’s fears about going to offices and classrooms because they have immunocompromised family members or young children at home who cannot be vaccinated. The risks are real. My husband has a condition that puts him at higher risk of hospitalization or death if he were to get COVID-19. I get it.
Each of us must do daily risk assessments to determine what risks we will tolerate. I shop for groceries in person (masked) rather than having them delivered, but I have not been to a restaurant except for takeout since March 2020. This week, I’ve been in a retreat with masked people, and the other day, I spoke with students (wearing masks) in a classroom. Some people may have gone to restaurants or the beach but are uncomfortable in a classroom. We make all sorts of trade-offs every day.
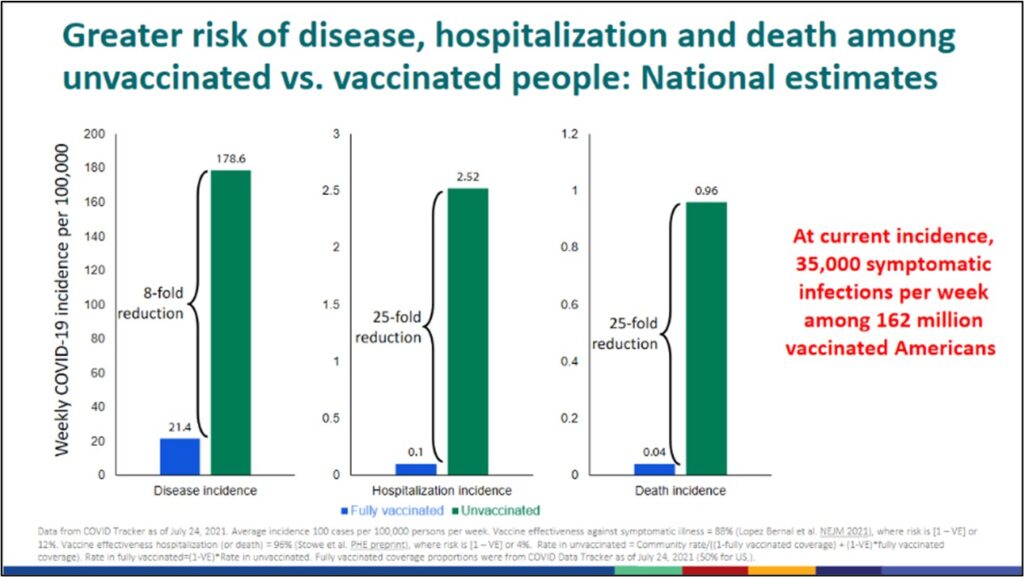
Data may help us to gain better insights into reasonable and unreasonable risks. Except for a small number of people with medical contraindications, being unvaccinated is one of the biggest risks for getting COVID-19. Or turn that around: getting vaccinated is one of the best protectors (see CDC chart below, based on data from COVID Tracker as of July 24, 2021).
The authorized vaccines aren’t perfect, but they are really good. Combining vaccination and a mask indoors offers great protection, but again, nothing is 100%. In our school, we are taking extra measures to put more oomph on the avoidance side of the COVID ledger. For example, we’re following advice from CDC on managing gatherings and events to minimize transmission of the virus (see this link).
UNC-Chapel Hill recently increased expectations for faculty and staff, notifying the Carolina community in an Aug. 6 letter of the requirement to attest to vaccination and upload CDC COVID-19 Vaccination Record Cards or be subjected to regular testing. Students already had been required to do that. This policy will help to create a safer for all of us. It is not a mandate, but it has some elements of a mandate—it’s Mandate Lite.
With move-in and welcome events already under way on our campus, a vaccine mandate now may not prevent clusters of infection this month and next. A week before the Aug. 18 start of in-person classes, about 85% of students, 92% of faculty and 64% of staff had attested to being vaccinated (see N&O).
Along with vaccination, the best defense against infection, according to David Weber, MD, MPH, who spoke with the Gillings community in a webinar Aug. 12 [beginning ~27:52 on video], is for everyone — vaccinated or unvaccinated — when outside of home to consistently wear a tight-fitting mask indoors at all times and outdoors when 6 feet of distance cannot be maintained [~49:30 on video]. Dr. Weber is Sanders Distinguished Professor of Medicine and Pediatrics; Professor of Epidemiology; Associate Chief Medical Officer and Medical Director of Infection Prevention, UNC Medical Center. Dr. Weber recommends not eating with others indoors or in close proximity outdoors because of the need to remove masks to do so [~1:18:20 on video].
While consistent mask-wearing is highly effective for prevention, we also recognize that within our community there are faculty, staff and students who must seek accommodations to forgo certain in-person activities to protect themselves or members of their household from infection (for example, those who are unable safely to wear a mask or be vaccinated). We all must do everything we can do — and respect others’ needs to do what they must do — to protect ourselves and others in our families and communities.
Finding equanimity amid chaos and fear
How do we continue to co-exist with a virus that upends our life? Somehow, we must learn to achieve equanimity. Sunday mornings, while I am walking, I listen to the NPR program “On Being” with Krista Tippett as a kind of spiritual refresher for the week ahead. On Aug. 8, she spoke with author and meditation teacher, Sharon Salzberg. They talked about finding one’s way in the world during the pandemic and discovering equanimity. I encourage readers to read the transcript or listen to the podcast. It’s quite uplifting. Here’s an excerpt:
 Sharon Salzberg: Certainly, if I heard the word “equanimity,” long ago, I’d have thought, that’s really bizarre. What does that mean? And so many times, we think it means indifference, but it really doesn’t. It’s such a huge capacity of our hearts to see what we’re going through, to see what others are going through, and to just have this perspective of, there is change in life, and there is light in the darkness and darkness in the light. And we’re not avoiding pain, because some things just hurt. That’s fundamental. But we’re holding it in a way that it’s like the love is stronger than the pain, even. And then we can really be with things in a very, very different way.
Sharon Salzberg: Certainly, if I heard the word “equanimity,” long ago, I’d have thought, that’s really bizarre. What does that mean? And so many times, we think it means indifference, but it really doesn’t. It’s such a huge capacity of our hearts to see what we’re going through, to see what others are going through, and to just have this perspective of, there is change in life, and there is light in the darkness and darkness in the light. And we’re not avoiding pain, because some things just hurt. That’s fundamental. But we’re holding it in a way that it’s like the love is stronger than the pain, even. And then we can really be with things in a very, very different way.
Barbara